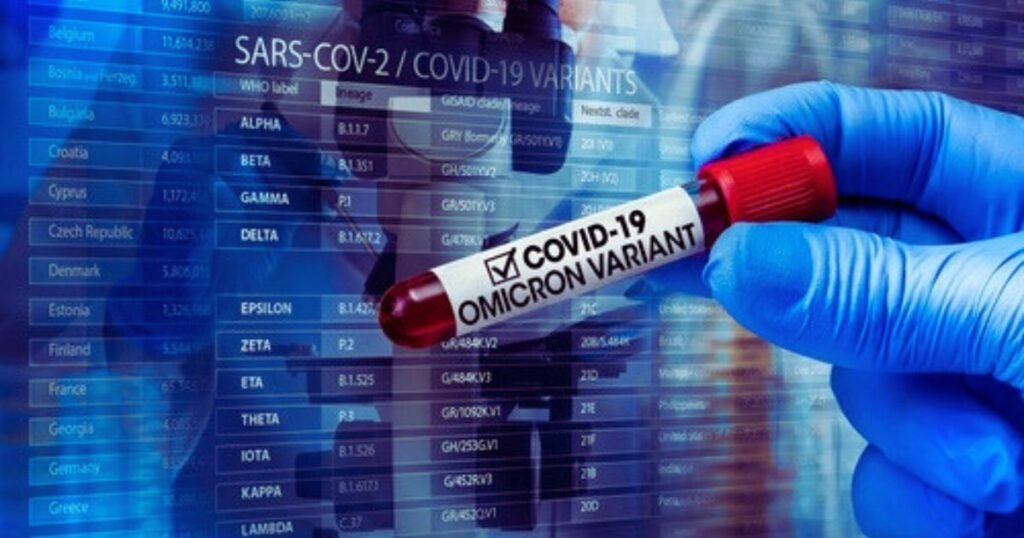
Introduction
As the COVID-19 pandemic extends into its fourth year, virologists anticipate the SARS-CoV-2 virus will continue evolving as all viruses do. COVID-19 Variants With still rampant spread globally, new variants certainly lie ahead. While most bring little overall change, the randomness of genetic mutations leaves open the possibility for future variants to emerge with altered traits like increased transmission, immune evasion to existing countermeasures, or virulence shifts. Maintaining vigilance through surveillance while planning smart public health responses allows proper preparation for future scenarios.
How New SARS-CoV-2 Variants Emerge
RNA viruses like SARS-CoV-2 continually accumulate genetic typos and mutations as they spread between hosts. Most random small mutations bring inconsequential changes. However, some chance errors alter viral characteristics in consequential ways – like a spelling change suddenly shifting word meaning. COVID-19 Variants Mutations enhancing transmission, disease severity, or immunity evasion offer the virus evolutionary advantages. Continued widespread infection provides more opportunities for such significant mutations to develop as replication cycles multiply in number.
Read More: Infectious Disease

Global Surveillance for Emerging COVID Variants
Thankfully robust tracking systems monitor COVID mutations worldwide. Researchers upload millions of viral sequences to global databases tracking lineages and characteristic genetic patterns. Sophisticated computational tools scan sequences looking for mutation clusters or regional distribution shifts that require further investigation.
The WHO designated certain major variants as variants of concern like Delta and Omicron which show clear public health impacts from changed traits. Lesser variants of interest also bear close observation for shifting properties. Careful monitoring provides early warning signs if new variants start dominating spread locally or internationally due to advantageous traits.
Concerning COVID Mutation Patterns
While intrinsic genomic instability ensures variants continue arising, practical traits determine their significance:
- Increased transmissibility – Mutations enhancing viral cell entry, replication rates inside cells, environmental stability, or particle concentrations in the respiratory system make respiratory spread more likely.
- Immune evasion – Accumulating spike protein mutations decreasing antibody binding from past infection or vaccines may enable reinfection or reduced vaccine efficacy over time.
- Altered disease severity – Some genetic changes may shift typical infection courses or complications. For example, Delta elicited more rapid respiratory decline in some groups.
- Assay interference – Certain mutations could reduce detection by standard PCR tests by affecting primer or probe binding sites.
Only expansive sequencing provides enough data to detect such patterns early when still regional.
What Perpetuates New COVID-19 Variants?
New viral strains arise from sustained viral reproduction. Until transmission drops dramatically either by infection or vaccination derived immunity, variants remain likely. Continued mutation drivers include:
- Animal reservoirs in species like mink, deer, allowing zoonotic spread
- Suboptimal global vaccination enabling spread in low immunity populations
- Waning natural and vaccine immunity over months/years
- Residual seasonal spread among partially immune groups
- Global travel quickly diffusing new strains before containment responses
Future mutations leading to new strains will continue arising from residual spread and reinfections as protection wanes without periodic boosting.
Readiness Planning for Potential Future Variants
While no one can predict if or when a variant might emerge rendering current protections less effective, preparedness strengthens response capacity. COVID-19 Variants Readiness steps include:
- Enhancing genomic surveillance globally for early alerts on trait changes
- Stockpiling variant-adjustable vaccine platforms and antiviral medications
- Simulating potential pandemic scenarios to set response requirements
- Bolstering medical supply reserves and hospital capacity where lacking
- Developing prototype vaccine boosters targeting likely viral mutations
- Ensuring flexibility to rapidly authorize updated treatments
- Aligning policymakers to allow science-guided actions
- Planning public communication surrounding future risks and response
With coordinated efforts and infrastructure built in recent years, the world can respond smarter if future variants warrant non-pharmaceutical interventions, treatments, or vaccine changes.
Conclusion
Virologists anticipate SARS-CoV-2 will continue evolving as long as substantial spread persists, prompting new viral lineages to emerge periodically. While impossible to entirely predict effects of random mutations, maintaining vigilance for early signals empowers public health authorities to respond appropriately based on viral traits that influence transmissibility, disease severity, and immunity evasion. By bolstering viral sequencing COVID-19 Variants efforts and planning infrastructure globally, future COVID variants can be handled in a deliberate fashion to minimize societal disruption. Pandemic responses rely on continuing science-informed actions coordinated compassionately across nations.
Read More: COVID-19 Variant

FAQs:
How often do new potentially risky COVID variants emerge?
Only a dozen or so highly concerning variants have arisen thus far warranting designated variant of concern status. COVID-19 Variants But lower risk variants of interest surface more routinely though location and impacts remain limited.
Can COVID become resistant to current vaccines over time?
Yes cumulative mutations, like those seen in Omicron’s offspring, can modestly erode vaccine protections for infection though COVID-19 Variants serious illness prevention holds up longer term. Periodic boosters with updated shots minimizes this risk.
When do new COVID variants become globally problematic?
Large case clusters or unusual clinical trends prompt investigation of new strains. Those demonstrating easier transmission spread internationally before contained. Global genomic COVID-19 Variants surveillance aims to detect signals weeks to months before widespread emergence.
Could new variants ever make COVID as deadly as originally?
Potentially but less likely. Viral evolution favors strains eliciting asymptomatic transmission over excessive lethality which curtails spread via serious illness. But virulence shifts remain COVID-19 Variants unpredictable long term.
What is the World Health Organization’s role with new variants?
WHO designates and names global variants of concern, releases recommended countermeasures, coordinates data sharing between countries, models future scenarios and monitors vaccine protections against emerging strains.