Introduction
Alcoholic fatty liver disease (AFLD) refers to a buildup of fat in the liver due to excessive alcohol use. It’s the earliest stage of alcoholic liver disease. While simple fatty liver may cause no damage, it can lead to more serious inflammatory conditions like alcoholic hepatitis and cirrhosis. Understanding AFLD risk factors, progression, diagnosis, and treatment steps empowers those battling alcohol addiction to halt further liver injury in time.
Who’s at Risk for AFLD?
Consuming more than 3 alcoholic drinks daily for women and 4 for men over months to years often causes fatty buildup. Genetics also influence sensitivity – Hispanics and Native Americans face higher risk. Fatty Liver Disease Being overweight or obese, consuming a high fat, high sugar diet, having diabetes or high triglycerides also increase AFLD likelihood.
Read More: Human Digestive System
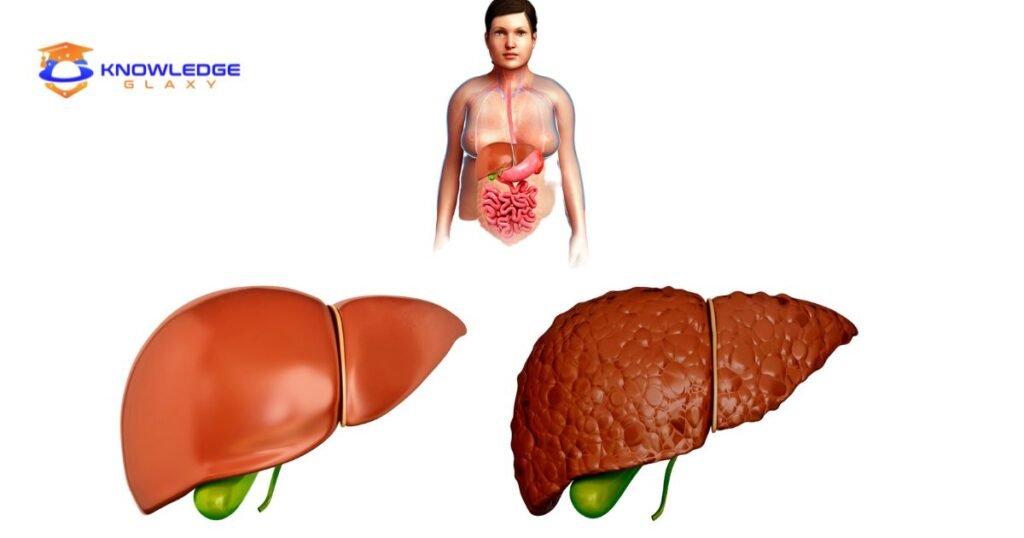
Given most drinkers meet one or more criteria, simple fatty liver is widespread, affecting over 90% of those who drink more than 16 g alcohol daily. Fortunately, early detection and alcohol cessation can prevent progression to permanent damage.
What Happens in Alcoholic Fatty Liver Disease?
Some alcohol metabolism generates free fatty acids and reactive oxygen species that drive fat production and inflammation in liver cells. Alcohol also impairs fat export from the liver. Over months to years, fat accumulates inside liver cells and ducts. This steatosis distends and weakens cells, impeding the liver’s ability to remove Fatty Liver Disease toxins from blood, metabolize nutrients, produce proteins, and regulate hormones. Though no fibrosis scar tissue forms initially, continued heavy drinking can trigger swelling and collagen scarring as cells die off, leading to alcoholic hepatitis. About 10-35% of individuals with long term AFLD eventually develop cirrhosis.
Signs and Symptoms Early
AFLD causes no symptoms as liver cells continue functioning despite fat. Without biopsy confirmation, most cases go undetected. Mild enlarged liver or discomfort in the upper right abdomen sometimes prompt detection. Bloodwork may reveal elevated liver enzymes AST and ALT. Only with inflammation is appetite and weight loss evident. Fatty Liver Disease Jaundice, fluid accumulation, easy bruising, mental confusion indicate advanced disease once extensive scarring has occurred.
Diagnosing Alcoholic Liver Disease
Since AFLD is often asymptomatic until late stages, diagnosis requires:
- Alcohol use history – Quantity, frequency, and duration to determine risk
- Physical exam – Doc notes enlarged, tender liver edge
- Blood tests check liver function through enzymes AST, ALT, GGT. Levels may lag behind histological disease.
- Ultrasound reveals fat visualizing the liver’s texture. Reads often appear normal early on.
- MRI scans can quantify liver fat when ultrasound is inconclusive.
- Liver biopsy definitively diagnoses AFLD severity looking at fat droplets and cellular changes.
Once AFLD is caught early, the best treatment is simply alcohol abstinence allowing the liver to fully recover.
Reversing Alcoholic Fatty Liver Disease Thankfully,
AFLD is initially reversible if alcohol is soon stopped before fibrosis sets in. Within weeks of sobriety, liver fat and enzymes generally normalize. Ensuring proper nutrition supports rapid liver cell regeneration. Key steps include:
- Quitting alcohol fully allows liver to metabolize fat again
- Following doctor’s health recommendations
- Correcting nutritional deficiencies through a balanced diet
- Managing diabetes and high blood fats if present
- Trying medications that reduce liver fat content
- Joining alcohol support groups and addiction counseling
- Having follow up bloodwork and scans to confirm improvement
Relapsing into heavy drinking can quickly reaccumulate fat and precipitate hepatitis. Thus sustained lifestyle changes are essential. With diligent sobriety, most fatty livers resolve without chronic damage.
Preventing AFLD Progression
Catching AFLD early and maintaining abstinence prevents progression to hepatitis and cirrhosis. Warning signs of advancing disease include fluid retention, jaundice, confusion, bruising easily, spiderlike blood vessels on skin, enlarged spleen, and liver Fatty Liver Disease scarring on biopsy. Without alcohol cessation, AFLD follows this damaging course in many patients:
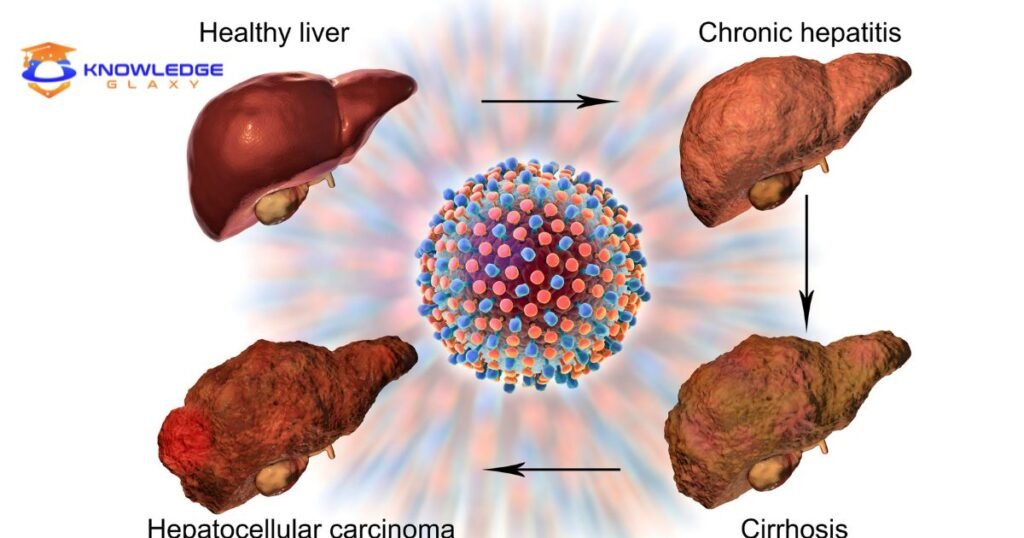
- Simple fatty liver ->
- Alcoholic hepatitis with necrosis and inflammation ->
- Fibrosis scarring ->
- Micronodular cirrhosis
Advanced cirrhosis causes internal bleeding, fluid buildup, toxin accumulation, liver cancer risk, and often irreversible organ damage warranting transplant. Fortunately, quitting drinking at any stage halts further damage. Even with cirrhosis, abstinence helps the liver regenerate some functional capacity.
Conclusion:
Intervene Early Catching alcoholic fatty liver disease early and stopping alcohol use promptly lets the liver recover fully before permanent structural damage sets in. Physicians have greater success motivating necessary lifestyle changes when caught in the reversible AFLD phase rather than late stage cirrhosis with poor prognosis. Successful recovery involves collaboration among physicians, therapists, social workers, addiction specialists and families/friends to help enable sobriety on every front. With today’s integrative treatment models and sustained vigilance, those battling alcohol addiction can reverse AFLD before it’s too late.

Read More: Alcoholic Fatty Liver Disease
FAQs
Does fatty liver go away once you stop drinking alcohol?
Yes, abstaining from alcohol gives the liver a chance to fully metabolize fat again with a return to normal texture in 91-100% of individuals if caught early before scarring.
What are the first signs my drinking is harming my liver?
Signs like upper right abdominal discomfort, fatigue, nausea can occur but often fatty liver causes no obvious symptoms initially. Blood work detects changes first.
Can I reverse alcoholic liver disease with lifestyle changes alone?
Yes, if caught early as simple fatty liver, stopping alcohol consumption combined with a healthy diet and active lifestyle enables full reversal in most patients.
What medications treat alcoholic liver disease?
No medications specifically target AFLD. Stopping alcohol while addressing nutrition deficiencies allows the liver to heal. Steroids help advanced alcoholic hepatitis.
How quickly can the liver recover after stopping drinking?
Recovery begins within days to weeks of sobriety depending on the degree of damage. Mild AFLD can normalize within 4-6 weeks with alcohol cessation and proper nutrition.