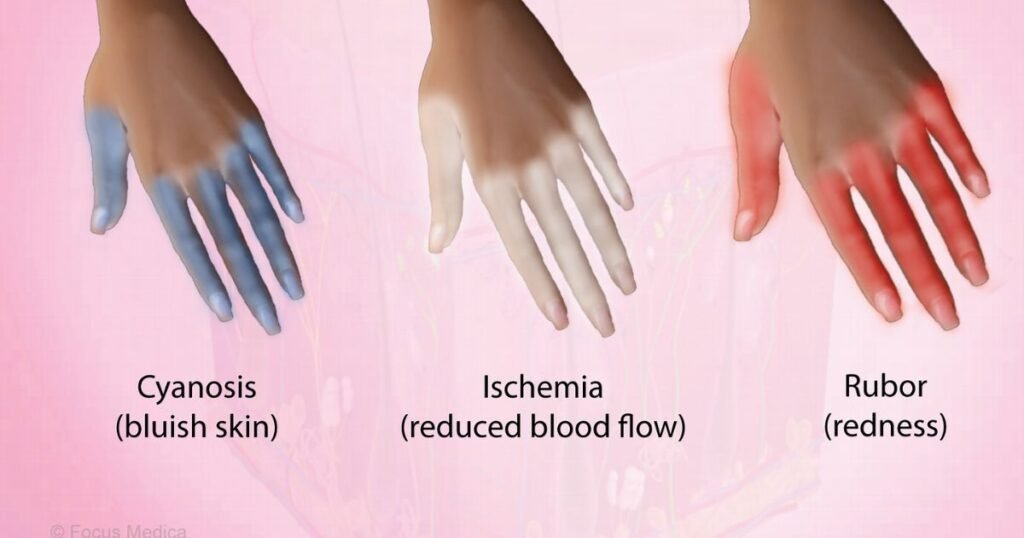
Raynaud’s is a condition in which the blood flow to the fingers and toes becomes restricted, often in response to cold or stress. It is an extremely painful condition, which can cause the fingers and toes to turn white and/or blue, to go numb, and to turn red and painful when blood flow returns. syndrome is a condition in which blood vessels spasm in response to cold or emotional stress. This condition can cause blood to be cut off from the surface of the skin, and this can lead to an erythema or discoloration of the affected area. Symptoms can range from mild to severe.
Raynaud’s phenomenon, also known as disease, is a medical condition that causes extreme sensitivity of the fingers, toes, and other parts of the hands and feet to cold. It is believed to be a disorder of the blood vessels in the extremities. Symptoms of are cold, blue, or white fingers or toes that may feel painful when exposed to cold temperatures or when exposed to stress. syndrome, a condition that affects blood circulation, causes the skin to turn white and blue when exposed to cold, making it painful to touch. The most common symptom of is the inability to feel the pulse in the fingers and toes.

Are you frequently experiencing cold and numb fingers and toes? Do you notice a change in the color of your skin when exposed to cold temperatures or stress? If so, you might be suffering from phenomenon, a condition that affects blood flow to the extremities. In this comprehensive article, we will explore the various aspects of including its symptoms, causes, and treatment options. Whether you are seeking answers for yourself or a loved one, read on to gain a deeper understanding of this condition and how to manage its impact on daily life.
A Brief Overview
Raynaud’s phenomenon, commonly referred to as is a condition characterized by vasospasms, which are episodes of narrowed blood vessels that limit blood flow to the extremities, such as the fingers and toes. This reduction in blood flow causes the affected areas to turn white, blue, and then red as the blood flow returns. These episodes, known as Raynaud’s attacks, can be triggered by exposure to cold temperatures or emotional stress.
Symptoms of Raynaud’s
Read More: Gene expression
Recognizing the symptoms of Raynaud’s is crucial in obtaining a timely diagnosis and appropriate treatment. The most common signs and symptoms include:
- Color changes in the skin: During a attack, the skin of the affected areas may turn white, then blue, and finally red as the blood flow returns.
- Numbness or tingling: Individuals with Raynaud’s may experience a sensation of numbness, tingling, or a “pins and needles” feeling in their fingers or toes.
- Cold extremities: The affected areas, such as the fingers and toes, often feel cold to the touch even in mild temperatures.
- Pain or discomfort: Raynaud’s attacks can be accompanied by pain, throbbing, or aching sensations in the affected areas.

Types of Raynaud’s
1. Primary Raynaud’s
Primary Raynaud’s, also known as disease, is the most common form of the condition. It typically develops gradually and does not have an underlying medical condition as its cause. Primary is often milder than the secondary form, and its exact cause is not well understood.
2. Secondary Raynaud’s
Secondary Raynaud’s, also referred to as phenomenon, is associated with an underlying medical condition. It tends to appear later in life and may have more severe symptoms compared to primary Some of the medical conditions that can cause secondary include:
- Connective tissue diseases: Conditions such as lupus, scleroderma, and rheumatoid arthritis can increase the risk of developing secondary.
- Vascular diseases: Disorders affecting blood vessels, including atherosclerosis and Buerger’s disease, can lead to secondary.
- Injuries: Trauma or repetitive injuries to the hands or feet can contribute to the development of secondary.
- Certain medications: Some medications, such as beta-blockers and certain chemotherapy drugs, may cause seconders as a side effect.
Causes of Raynaud’s: Unraveling the Factors
Understanding the underlying causes of Raynaud’s can shed light on the condition and help individuals manage its impact more effectively. While the exact cause of primary remains unknown, several factors contribute to the development of both primary and secondary. Let’s explore these causes in more detail:
Dysfunction in blood vessel response
One of the primary factors contributing to is believed to be an abnormal response in the blood vessels. In individuals with the blood vessels in the fingers and toes overreact to certain triggers, leading to vasospasms and reduced blood flow. This abnormal response is thought to be influenced by both genetic and environmental factors.
Cold temperatures and stress
Cold temperatures and emotional stress are common triggers for Raynaud’s attacks. Exposure to cold can cause blood vessels to constrict, reducing blood flow to the extremities and triggering an episode. Similarly, emotional stress or anxiety can lead to an increased release of stress hormones, which can further contribute to vasospasms.

Gender and age
Raynaud’s is more prevalent in women compared to men, with the condition typically appearing between the ages of 15 and 30. Hormonal factors may play a role in this gender disparity, as hormonal changes can affect blood vessel response. Additionally, older individuals are more likely to develop secondary due to the increased prevalence of underlying medical conditions associated with the condition.
Smoking and caffeine consumption
Smoking and excessive caffeine intake have been linked to an increased risk of developing Raynaud’s and worsening its symptoms. Both smoking and caffeine can constrict blood vessels and impair circulation, exacerbating the effects of attacks.
Occupational factors
Certain occupations that involve prolonged exposure to cold temperatures or the use of vibrating tools increase the risk of developing Raynaud’s. Individuals in professions such as construction, fishing, and manufacturing may be more susceptible to the condition.
Diagnosing Raynaud’s: Identifying the Condition
If you suspect that you or someone you know may have Raynaud’s, it is essential to seek medical attention for a proper diagnosis. A healthcare professional, often a rheumatologist or a dermatologist, will evaluate the symptoms and medical history to determine if is the underlying cause. The diagnosis typically involves:
- Physical examination: The doctor will examine the affected areas and assess the color changes and other visible symptoms during an episode.
- Medical history review: The doctor will inquire about the frequency and duration of attacks, as well as any other medical conditions or medications that may contribute to the condition.
- Blood tests: Blood tests may be conducted to rule out underlying medical conditions associated with secondary, such as autoimmune disorders.
- Cold challenge test: In some cases, a cold challenge test may be performed to provoke a attack and observe the response of the blood vessels.
Managing Raynaud’s: Tips for Coping with the Condition
While there is no cure for various strategies and lifestyle modifications can help manage the condition and reduce the frequency and severity of attacks. Consider implementing the following tips to cope.
1. Stay warm and layer clothing
Keeping warm is essential for individuals with Raynaud’s. Dressing in layers allows you to adjust your clothing to the temperature and provides better insulation. Wearing gloves, warm socks, and thermal shoes can help maintain warmth in the extremities.
2. Protect your hands and feet
During cold weather or when handling cold objects, protect your hands and feet by wearing mittens or gloves and insulated footwear. Additionally, using hand warmers or heated insoles can provide extra warmth when needed.

3. Avoid triggers
Identify and avoid triggers that may provoke attacks. If cold temperatures trigger your symptoms, try to limit your exposure by staying indoors or using heated spaces. Similarly, managing stress through relaxation techniques or counseling can help reduce the impact of emotional triggers.
4. Regular exercise
Engaging in regular physical activity promotes circulation and helps maintain overall cardiovascular health. Incorporate exercises that improve blood flow, such as aerobic activities, into your routine. However, be mindful of exercising in extreme temperatures, as it may trigger attacks.
5. Quit smoking and reduce caffeine intake
If you smoke, quitting is highly recommended for managing Raynaud’s symptoms. Smoking constricts blood vessels and impairs circulation, exacerbating the condition. Additionally, limiting your caffeine intake can help reduce the frequency and severity of attacks.
6. Medication options
In severe cases, medication may be prescribed to manage symptoms. Calcium channel blockers, such as nifedipine, can help relax and widen blood vessels, improving blood flow. Other medications, including alpha blockers and vasodilators, may also be prescribed in specific situations.
It’s important to consult with a healthcare professional to determine the most suitable treatment plan for your individual needs.
Read More: Raynaud’s disease
FAQs about Raynaud’s
Q1. Is Raynaud’s a serious condition?
Yes, Raynaud’s can be a serious condition, especially when it is secondary to an underlying medical condition. It is essential to manage the condition properly to prevent complications and minimize the impact on daily life.
Q2. Can stress worsen Raynaud’s symptoms?
Yes, stress can worsen Raynaud’s symptoms. Emotional stress or anxiety can lead to an increased release of stress hormones, which can further constrict blood vessels and trigger attacks.
Q3. Can Raynaud’s affect other parts of the body besides the fingers and toes?
While primarily affects the fingers and toes, it can also affect other areas such as the nose, ears, lips, and nipples. These areas may experience color changes and reduced blood flow during episodes.
Q4. Can Raynaud’s be cured?
Currently, there is no cure for Raynaud’s. However, with appropriate management and lifestyle modifications, most individuals can effectively control the condition and reduce the frequency and severity of attacks.
Q5. Can Raynaud’s be prevented?
While cannot be prevented entirely, certain lifestyle modifications can help reduce the risk of developing or manage its symptoms. These include avoiding triggers, maintaining warmth, and practicing stress management techniques.
Q6. Can Raynaud’s lead to complications?
In some cases, can lead to complications such as skin sores or ulcers, infections, or, rarely, tissue damage. These complications usually occur in severe cases or when is secondary to an underlying medical condition.
In Conclusion
Raynaud’s phenomenon is a condition that affects blood flow to the extremities, causing episodes of color changes and discomfort in the fingers and toes. While there is no cure, individuals with can effectively manage the condition and reduce its impact on daily life. By implementing lifestyle modifications, avoiding triggers, and seeking appropriate medical treatment, individuals can experience improved quality of life and minimize the frequency and severity of attacks.
Remember, if you suspect you have or are experiencing concerning symptoms, it is important to consult with a healthcare professional for an accurate diagnosis and personalized treatment plan. With proper care and management, individuals with can lead fulfilling and comfortable lives.